Scaphoid non-union
Scaphoid fractures have a bad reputation, which is fairly well deserved (see scaphoid fractures).
When a scaphoid fracture fails to heal, the result is called a non-union, or pseudarthrosis (which means “false joint”). What you are left with is a bone with a gap where the fracture was, containing fibrous tissue (or “grissle” in layman’s terms).
The non-union leads to shortening of the bone and a flexed shape through the gap in the bone. This change in shape is what alters the wrist mechanics, and leads to premature cartilage deterioration in the wrist. This leads to wrist arthritis, known in this case as SNAC wrist (scaphoid non-union advanced collapse).
Once there is an established non-union, only surgery can achieve healing. Surgery should be considered if a scaphoid non-union has been identified, and there are no severe arthritic changes present in the wrist.
In treating scaphoid non-unions, the bone ends must be freshened, the shape corrected, the defect filled with bone graft and the construct stabilised with internal fixation.
Traditional open surgery with bone graft and a compression screw leads to healing 80% of the time. Open surgery means opening the bone to the outside, with a generous skin incision and an “open approach”. The problem with the open approach is that it must further injure the blood supply of the scaphoid, which was one of the factors that lead to the problem in the first place.
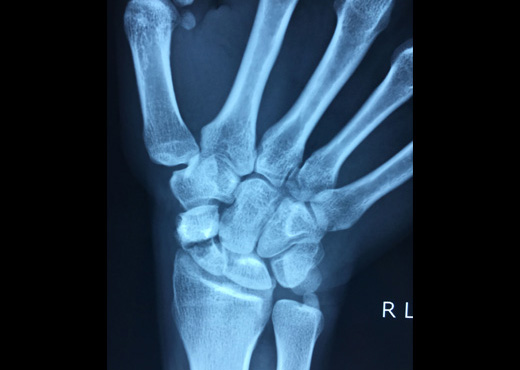
X-ray of a scaphoid waist non-union
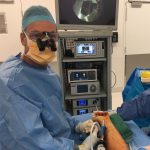
Arthroscopic video of bone graft insertion
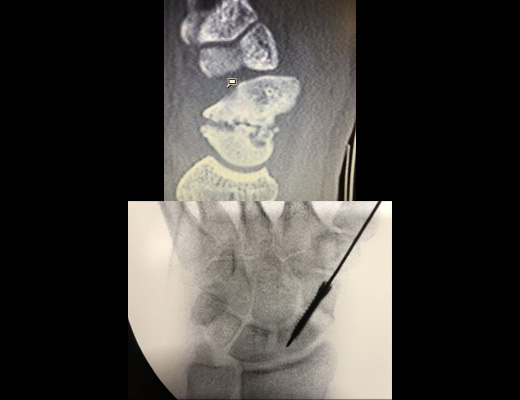
Top: CT scan of scaphoid non-union with “humpback deformity”, Bottom: correction of deformity with neutralisation screw
Healing rates have been improved by using “vascularised” bone graft, that is bone grafts with their own artery and vein. Using microsurgical techniques, vascularised bone grafts from the inside of the knee lead to healing rates of up to 95%. However, this is fairly invasive surgery, with extensive approaches required and the possibility of significant problems around the knee. There is also usually a degree of permanent wrist stiffness afterwards from the more extensive dissection.
Arthroscopic bone grafting (ABG) is my preferred technique for dealing with most scaphoid non-unions. Reported healing rates are 95-100%, which has been my experience also. The surgery is performed through 3mm arthroscopic portals, with a 10mm incision over the iliac crest to harvest cancellous (spongey) bone graft. It is probable that it is the less invasive nature of this form of surgery which leads to such high rates of healing. The blood supply of the scaphoid is minimally affected by the surgery.
Arthroscopic bone grafting of scaphoid non-unions was originally described with smooth pin (K-wire) fixation. Whilst this is fine when there is minimal deformity through the non-union, it may be insufficient to correct “humpback” deformities. These wires also require a second surgery for removal, and wrist motion must be delayed until healing is advanced enough to allow wire removal.
In looking to advance the results from scaphoid ABG, some improvement in the fixation seemed a good starting point. Ideally, the fixation is still minimally invasive (percutaneous), can hold correction of the shape and is strong enough to allow earlier motion of the wrist. I have pioneered the use of “neutralisation” screw fixation, in conjunction with ABG for scaphoid non-unions. The surgery is largely the same as previously, but the scaphoid deformity is corrected and fixed with the screw before the bone graft is inserted into the defect (see photos). The outcomes with this technique have been very gratifying, in terms of speed of bone healing and return of motion.
After arthroscopic bone grafting and neutralisation screw fixation, the patient wears a splint for 6 weeks. A CT scan is then performed to check the bone graft is incorporating, and then motion exercises are commenced. A further CT scan is performed at 12 weeks prior to returning to normal activities, if healing is adequately advanced, which it normally is at that stage.
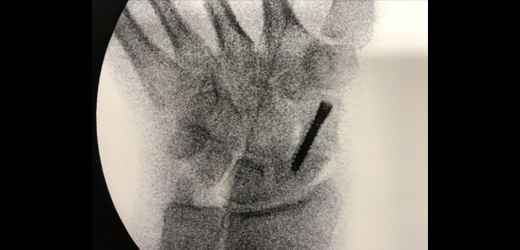
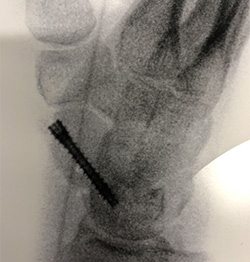

Top & bottom left: X-rays following correction of deformity with neutralisation screw and bone grafting (arthroscopic), Bottom right: newclip technics neutralisation screw, designed by Dr Nicholas Smith